How infectious diseases are spread and simple and practical advice for preventing the spread of infection in the home and community
Anthrax - including symptoms, treatment and prevention
Anthrax is an acute infectious disease caused by bacteria called Bacillus anthracis. The anthrax bacterium produces spores (small resistant cells) which are capable of surviving for many years in the environment. Anthrax most commonly occurs in wild or domesticated warm-blooded grazing animals such as sheep and cattle, but can infect humans.
Anthrax is a notifiable condition1
How anthrax spreads
Anthrax is a very rare disease in Australia, and usually occurs in farmers or other people who have close contact with animals or their products, especially wool, animal hair or skins. Infection can involve the skin if the bacteria enter a cut or abrasion. Infection can also occur if spores are inhaled or if meat from an infected animal is eaten.
Anthrax is a potential agent for use in biological warfare.
Signs and symptoms of anthrax
Symptoms of anthrax vary depending on how the disease was contracted.
Cutaneous anthrax
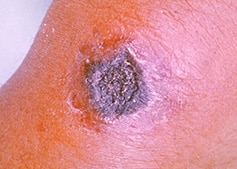 Cutaneous anthrax is anthrax initially involving the skin. It begins as a raised itchy bump resembling an insect bite, which then develops into a vesicle (blister), then into a painless ulcer with a characteristic black area in the centre (see image). There is usually marked swelling around the area and lymph glands in the adjacent area may swell. Up to 20% of untreated people may die. Deaths from cutaneous anthrax are rare with appropriate antibiotic treatment.
Cutaneous anthrax is anthrax initially involving the skin. It begins as a raised itchy bump resembling an insect bite, which then develops into a vesicle (blister), then into a painless ulcer with a characteristic black area in the centre (see image). There is usually marked swelling around the area and lymph glands in the adjacent area may swell. Up to 20% of untreated people may die. Deaths from cutaneous anthrax are rare with appropriate antibiotic treatment.
Image courtesy Public Health Image Library (PHIL), Department of Health and Human Services, Centers for Disease Control and Prevention (CDC-USA)
Inhalational anthrax
Inhalational anthrax may occur when spores are breathed in. Inhalation anthrax may initially resemble flu-like illness, but after several days severe breathing problems and shock may develop. Without treatment, death usually occurs 1 to 2 days after the onset of severe symptoms.
Intestinal anthrax
Intestinal anthrax may occur following eating contaminated meat. Symptoms may include: nausea, loss of appetite, vomiting, fever, abdominal pain, vomiting of blood and severe diarrhoea. Up to 60% of people with intestinal anthrax will die without treatment.
Diagnosis of anthrax
Anthrax is usually diagnosed by isolating Bacillus anthracis from the blood, skin lesions or respiratory secretions.
Incubation period
(time between becoming infected and developing symptoms)
Usually 1 to 7 days, but can be up to 2 months.
Infectious period
(time during which an infected person can infect others)
Person-to-person transmission of anthrax is very rare and has been reported only with cutaneous anthrax.
Articles and soil contaminated with anthrax spores may remain infective for decades.
Treatment for anthrax
Treatment with antibiotics is essential, particularly for inhalational anthrax. In some situations preventative antibiotics may also be given to people who are suspected to have been exposed to anthrax spores.
Prevention
- Control of anthrax in livestock herds is essential for prevention of its spread to humans. Animals dying from anthrax usually die suddenly, with only a brief illness preceding death. By law, a farmer who suspects anthrax in an animal must notify a government veterinary officer immediately. If anthrax is suspected the farm will be isolated and herds vaccinated, and the dead animal disposed of appropriately so that contamination of the soil is minimised.
- Anthrax vaccines exist for use in livestock in Australia, but are not currently registered for use in humans. They have been used for protection of military personnel who are considered to be at risk of exposure to biological weapons.
- Safety regulations covering rendering plants and factories processing wool and hides must be adhered to. Workers should also wear protective clothing.
- Even a single case of human anthrax is so unusual in Australia that it should be reported urgently to public health authorities. Anthrax spores have been used in bioterrorist attacks in the United States of America and it is important that sources of any infections are identified quickly so that control measures may be put into place.
Useful links
1 – In South Australia the law requires doctors and laboratories to report some infections or diseases to SA Health. These infections or diseases are commonly referred to as 'notifiable conditions'.
Image - Anthrax lesion on the skin of the forearm Image courtesy Public Health Image Library (PHIL) Department of Health and Human Services Centers for Disease Control and Prevention (CDC-USA)